Retina Disease
Protecting the Most Delicate Part of Your Vision
Understanding about Retina
The retina is a light-sensitive layer of tissue lining the back of the eye that plays a crucial role in vision. Often compared to the film in a camera, the retina captures light images focused by the cornea and lens, converts them into electrical signals, and sends these signals through the optic nerve to the brain, where they are interpreted as vision. The retina contains millions of photoreceptor cells called rods and cones. Rods help with vision in low light conditions, while cones are responsible for color vision and fine detail. The most central part of the retina, called the macula, is responsible for sharp, detailed central vision needed for activities like reading and recognizing faces. When the retina is damaged or diseased, vision impairment occurs, ranging from minor visual disturbances to complete blindness, depending on the severity and location of the damage.
Types of Retina Disease
Diabetic Retinopathy
Damage to retinal blood vessels caused by long-term diabetes.
Macular Hole
A small break in the macula causing blurred central vision.
Hypertensive Retinopathy
Retinal damage due to uncontrolled high blood pressure.
Macular Edema
Swelling in the macula due to fluid leakage.
Retinal Detachment
The retina separates from the back of the eye — a medical emergency.
Retinopathy of Prematurity (ROP)
Abnormal retinal vessel development in premature infants.
Symptoms of Retina Disease
- Sudden blurred or distorted vision
- Floaters or dark spots
- Flashes of light
- Loss of central vision
- Loss of peripheral vision
- Straight lines appearing wavy
- Sudden shadow or curtain over vision
Causes of Retina Disease
- Diabetes
- High blood pressure
- Aging
- Eye trauma
- Genetic factors
- Inflammatory conditions
- Premature birth
- Retinal tears
Precautions

Blood Sugar & BP Control
Strict management slows progression.
Blood Sugar & BP Control
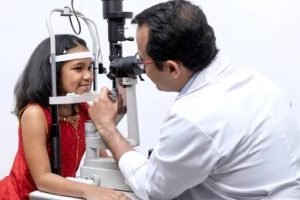
Regular Retina Screening
Essential for diabetic and high-risk patients.
Regular Retina Screening

Intravitreal Injections
Used for macular edema.
Intravitreal Injections
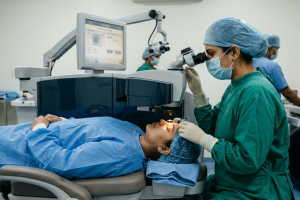
Laser Treatment
Prevents further leakage and vessel damage.
Laser Treatment
Retina Surgery Overview
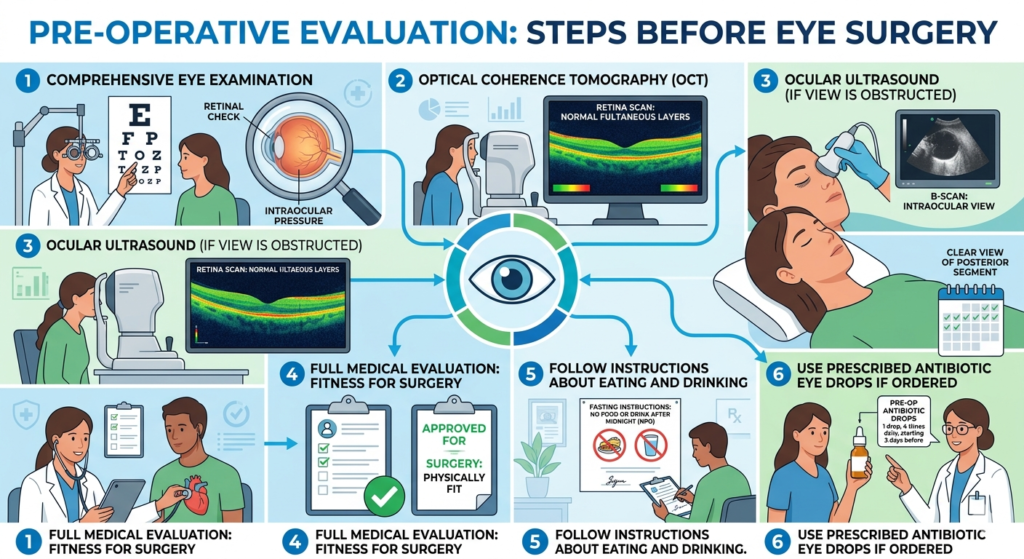
Before Retina Surgery
- Comprehensive eye examination.
- Optical coherence tomography (OCT).
- Ocular ultrasound if view is obstructed.
- Full medical evaluation to ensure fitness for surgery.
- Follow instructions about eating and drinking.
Use prescribed antibiotic eye drops if ordered.
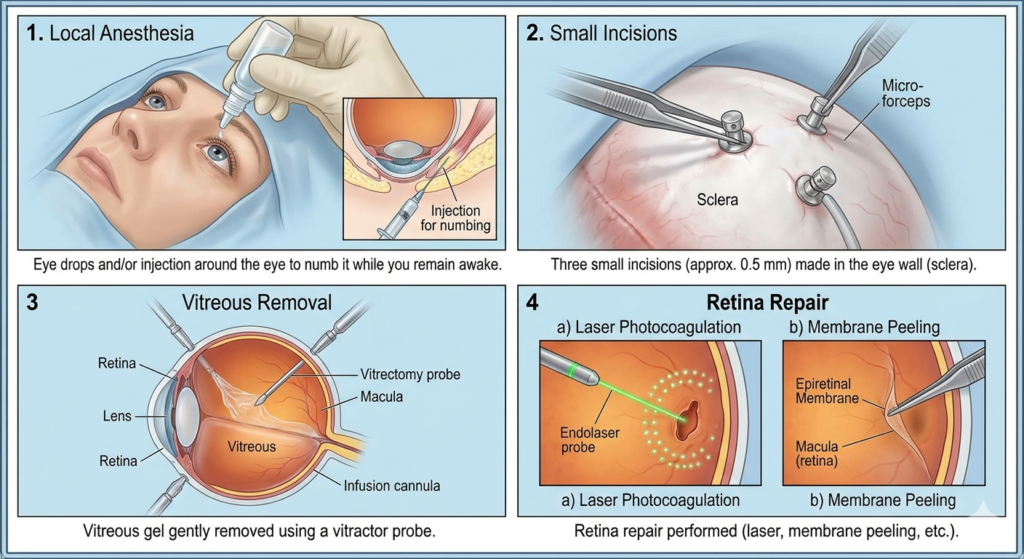
During Retina Surgery
- Local anesthesia: Eye drops and/or injection around the eye to numb it while you remain awake.
- Small incisions made in the eye wall.
- Vitreous gel gently removed.
- Retina repair performed (laser, membrane peeling, etc.)

After Retina Surgery
- Eye will be padded and shielded for protection
- Some discomfort, redness, or swelling is normal
- Vision will be blurry (especially with gas bubble).
- Avoid rubbing the eye.
No driving until vision clears and doctor approves
Treatments
Vitrectomy Surgery
- Small incisions (less than 1mm) are made in the eye wall to insert surgical instruments.
The vitreous gel is carefully removed to provide access to the retina for repair.
Specialized techniques like laser, membrane peeling, or retinal reattachment are performed during the procedure.
The surgery typically lasts 1-3 hours depending on the complexity of the case.
It is performed under local anesthesia with sedation or general anesthesia.
Air travel is strictly prohibited until any gas bubble completely absorbs.
- Success rates are high (80-90%) for conditions like retinal detachment
Anti-VEGF Injections (Intravitreal Injections)
Procedure involves injecting medication into the vitreous gel of the eye using a very fine needle.
Eye is numbed with anesthetic drops before injection to ensure patient comfort.
Common anti-VEGF drugs include Ranibizumab (Lucentis), Aflibercept (Eylea), and Bevacizumab (Avastin).
Treatment aims to stop abnormal blood vessel growth and reduce fluid leakage in the retina.
Injections are typically given at regular intervals (monthly or bi-monthly) based on the condition and response.
The procedure takes only a few minutes and is performed in an outpatient setting.
Patients may notice vision improvement within days to weeks after injection.
Most patients require a series of injections over months or years for optimal results.
Frequently Asked Questions
The retina is the light-sensitive layer at the back of the eye that captures images and sends them to the brain. It’s essential for vision, much like the film in a camera.
Sudden floaters (spots), flashes of light, dark curtain over vision, blurred or distorted vision (straight lines appearing wavy), and loss of central or peripheral vision.
YES. Retinal detachment is a medical emergency requiring immediate treatment within 24-48 hours to prevent permanent vision loss. If you experience sudden flashes, floaters, or a dark curtain over vision, seek emergency eye care immediately.
Many retinal conditions can be treated successfully, especially with early detection. Treatments include medications (injections), laser, and surgery. Some conditions can be managed but not cured, while others (like early-detected retinal detachment) can be fully repaired with good vision recovery.
It’s a complication of diabetes where high blood sugar damages blood vessels in the retina. These vessels may leak fluid, bleed, or grow abnormally, leading to vision loss. It’s the leading cause of blindness in working-age adults.
Type 1 diabetics should have dilated eye exam within 5 years of diagnosis, then annually. Type 2 diabetics should have exam at time of diagnosis, then annually. Pregnant diabetics should have exam during first trimester. More frequent exams may be needed if retinopathy develops.
- Age-related macular degeneration (AMD) affects the macula (central retina), causing loss of central vision used for reading, driving, and recognizing faces. It occurs in dry (slow-progressing) and wet (rapid-progressing with leaking vessels) forms.
Only when your vision meets legal requirements and your doctor approves. This is typically weeks to months after surgery, depending on the procedure and healing.
Many patients need glasses for optimal vision after retinal treatment, especially for reading. Final prescription is usually given 3-6 months after surgery when vision stabilizes.
1. Older Adults (Age 50+)
Increased risk of macular degeneration, retinal tears/detachment due to vitreous changes
2. Diabetic Patients
Leading cause of new blindness in adults; risk increases with duration of diabetes
3. High Myopes (Nearsighted -6D or greater)
Thinner retinas more prone to tears and detachment
4. Individuals with Family History
Genetic predisposition to macular degeneration, retinitis pigmentosa, retinal detachment
5. Patients with Eye Trauma History
Previous injury increases retinal tear/detachment risk
6. Post-Cataract Surgery Patients
Slight increased risk of retinal detachment, especially if complications occurred
7. People with Inflammatory Conditions
Uveitis, autoimmune diseases affecting eyes
8. Individuals with Cardiovascular Disease
Hypertension, atherosclerosis affect retinal blood vessels
9. Smokers
Significantly higher risk of macular degeneration
10. Premature Infants
Risk of retinopathy of prematurity (ROP)
11. People with Lattice Degeneration
Thin areas in peripheral retina prone to tears
12. Patients on Long-Term Certain Medications
Hydroxychloroquine, tamoxifen, and others can be toxic to retina
