Pediatric Ophthalmology Disease
Protecting Vision from the Very Beginning
Understanding about Pediatric Ophthalmology
Pediatric Ophthalmology is a specialized branch of medicine focused on eye care for children, from newborns through adolescents. This field addresses the unique visual needs of developing eyes, as children’s visual systems are still maturing until about age 8-10. During this critical period, any eye condition that interferes with clear vision can lead to permanent visual impairment if not treated early. Pediatric ophthalmologists are trained to diagnose, treat, and manage all eye problems affecting children, understanding that children are not simply small adults—their eyes require different approaches to examination and treatment.
TYPES OF PEDIATRIC EYE DISEASE
Squint (Strabismus)
Misalignment of the eyes where one eye may turn inward, outward, upward, or downward.
Congenital Cataract
Clouding of the lens present at birth.
Amblyopia (Lazy Eye)
Reduced vision in one eye due to improper visual development.
Retinopathy of Prematurity (ROP)
Affects premature infants due to abnormal retinal vessel development.
Refractive Errors
Near-sightedness, far-sightedness, or astigmatism in children.
Pediatric Glaucoma
Rare but serious condition affecting eye pressure in children.
Symptoms of Pediatric Eye Disease
- Eyes not aligned properly
- Frequent eye rubbing
- Squinting or head tilting
- Poor eye contact
- Sensitivity to light
- Excessive tearing
- White reflex in pupil
- Difficulty reading or focusing
Causes of Pediatric Eye Disease
- Genetic factors
- Premature birth
- Developmental abnormalities
- Infections during pregnancy
- Trauma
- Uncorrected refractive errors
Precautions

Prescription Glasses
Correct refractive errors and support proper vision development.
Prescription Glasses

Patching Therapy
Used in amblyopia to strengthen the weaker eye.
Patching Therapy

Vision Therapy
Exercises to improve coordination and focusing.
Vision Therapy

Regular Monitoring
Track development and prevent complications.
Regular Monitoring
Pediatric Eye Disease Treatment Overview

Before Surgery
- Pediatrician evaluation to ensure your child is healthy for surgery
- No food or drink for several hours before surgery
- Discussing current medications and whether any should be stopped.
- Planning for admission and post-operative care.
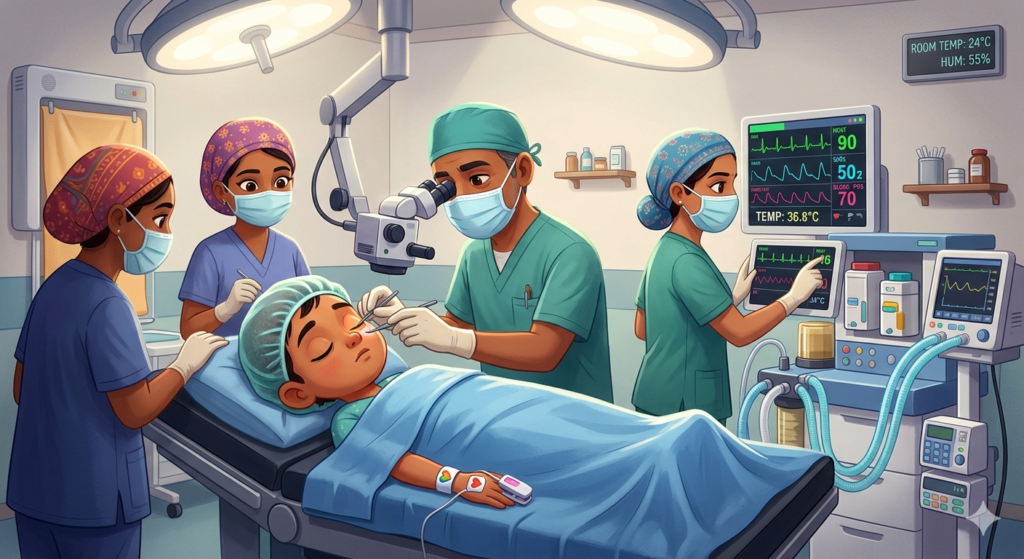
During Surgery
- Surgeries are performed under general anesthesia.
- This is to ensure the child remains completely still and comfortable throughout the procedure.
- Throughout surgery, the care team ensures temperature regulation, continuous monitoring.
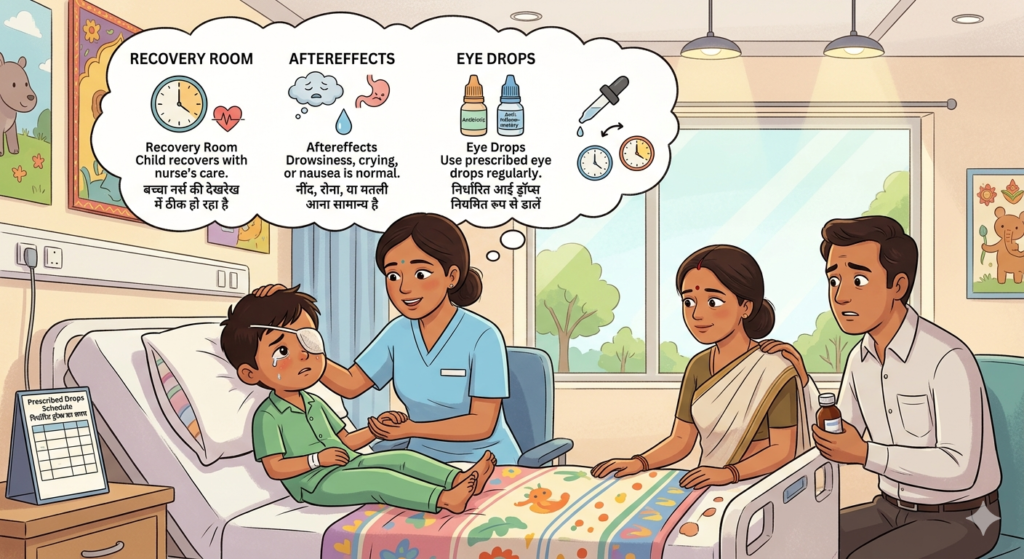
After Surgery
- Your child will wake up in the recovery room with nursing supervision.
- Some confusion, crying, or nausea is common as anesthesia wears off.
- Administer prescribed antibiotic and anti-inflammatory drops exactly as scheduled.
Frequently Asked Questions
Pediatric ophthalmology is a specialized field of medicine dedicated to eye care for children from birth through adolescence. It focuses on diagnosing and treating eye conditions that affect the developing visual system, understanding that children’s eyes are different from adults and require specialized approaches to examination, treatment, and follow-up care.
1. Amblyopia (Lazy Eye) – Reduced vision in one eye due to abnormal development
2. Strabismus (Crossed Eyes) – Misalignment of the eyes
3. Refractive Errors – Nearsightedness, farsightedness, astigmatism
4. Pediatric Cataracts – Clouding of the eye’s natural lens
5. Blocked Tear Ducts – Common in newborns causing watery eyes
6. Conjunctivitis (Pink Eye) – Infection or inflammation
7. Ptosis – Drooping upper eyelid
8. Retinopathy of Prematurity – Affecting premature infants
9. Color Vision Deficiency – Difficulty distinguishing colors
10. Eye Injuries – Trauma from accidents or sports
1. Newborn Period: All infants should have a red reflex test before hospital discharge
2. 6-12 Months: Comprehensive eye exam recommended, especially for high-risk infants
3. 3-4 Years: First comprehensive eye exam for all children
4. Before Kindergarten: Essential to ensure vision ready for learning
5. Annually: Regular exams through school years
6. Immediately: If any signs of eye problems appear at any age
7. Earlier for High-Risk Children: Premature infants, family history of eye problems, developmental delays
Yes, vision problems can significantly impact learning. Undetected eye conditions may cause:
Difficulty reading the board at school
Avoiding reading and close work
Short attention span for visual tasks
Headaches and eye strain during homework
Poor handwriting and copying skills
Difficulty with reading comprehension
Behavioral issues from frustration
Reduced participation in sports and activities
Misdiagnosis as learning disabilities or ADHD
80% of learning is visual, making regular eye exams essential for academic success.
Signs of healthy vision in infants include:
Birth to 3 Months:
Looks at faces and objects briefly
Begins to follow moving objects with eyes
Responds to bright light by blinking
3 to 6 Months:
Reaches for and grabs objects
Recognizes familiar faces at a distance
Eyes move together smoothly
6 to 12 Months:
Crawls toward objects of interest
Uses fingers to point at things
Shows interest in picture books
Warning Signs to Watch For:
Eyes don’t move together
Excessive tearing or sensitivity to light
White pupil in photos
Doesn’t make eye contact
Bumps into furniture after starting to walk
Always tilts head to one side
The optimal age for strabismus surgery depends on the type and cause:
Infantile Esotropia: Often between 6 months to 2 years for best binocular vision development
Intermittent Exotropia: Usually age 3-5 years or when deviation becomes frequent
Congenital Conditions: As early as medically safe
Acquired Strabismus: After treating underlying cause and stabilizing angle
Adult Strabismus: At any age for functional or cosmetic reasons
While myopia has genetic components, progression can be slowed:
Increase Outdoor Time: 1-2 hours daily outdoor activity reduces myopia risk
Reduce Screen Time: Follow 20-20-20 rule (20 second break every 20 minutes, looking 20 feet away)
Proper Reading Distance: Maintain at least arm’s length from books/screens
Good Lighting: Ensure adequate light for near work
Regular Eye Exams: Early detection allows intervention
Atropine Eye Drops: Low-dose drops may slow progression (doctor prescribed)
Orthokeratology: Special contact lenses worn overnight to reshape cornea
Multifocal Contact Lenses: Special designs that may slow progression
Outdoor Breaks: Especially important during prolonged near work
Balanced Diet: Nutrients supporting eye health
Preparation tips by age:
Infants and Toddlers:
Schedule during alert, happy times
Bring familiar comfort items
Feed before appointment
Bring favorite toy to focus attention
Preschoolers:
Explain using simple, positive words
Read books about visiting doctor
Play “eye doctor” at home
Bring sunglasses if light sensitive
Promise a small reward afterward
School-Aged Children:
Explain what to expect honestly
Assure them it doesn’t hurt
Discuss importance of good vision
Let them ask questions
Bring glasses if they wear them
General Tips:
Arrive early to avoid rushing
Bring snacks and water
Bring current glasses/contact lenses
Know family eye history
List any concerns or observations
1. Premature Infants: Higher risk of retinopathy of prematurity and refractive errors
2. Family History: Children with parents/siblings having strabismus, amblyopia, or high refractive errors
3. Developmental Delays: Children with neurological conditions or syndromes
4. Genetic Conditions: Down syndrome, Marfan syndrome, etc.
5. Maternal Infections During Pregnancy: Rubella, toxoplasmosis, CMV
6. Low Birth Weight Babies: Increased risk of various eye problems
7. Children with Systemic Diseases: Juvenile arthritis, diabetes
8. Medication Exposure: Certain medications during pregnancy or childhood
9. Head or Eye Trauma: Previous injuries increase risk
10. Children with Poor Nutrition: Especially lacking vitamin A
11. Excessive Screen Time: May accelerate myopia progression
12. Limited Outdoor Activity: Associated with higher myopia risk
