Corneal Ulcer Disease
Early Treatment Prevents Permanent Vision Damage
Understanding about Corneal Ulcer
Corneal ulcers are a serious eye condition where the normally clear cornea develops an open sore, leading to pain, redness, and potential vision loss. This condition can develop rapidly over hours to days and is often associated with infection, but it can also be caused by other factors such as trauma, contact lens overuse, or dry eyes.
Types of Corneal Ulcers
Fungal Keratitis
Fungal infection of the cornea, often after injury with plant material.
Corneal Scarring
Permanent scarring after untreated ulcers.
Bacterial Keratitis
Bacterial infection causing pain, redness, and discharge.
Keratoconus
Progressive thinning and bulging of the cornea affecting vision.
Viral Keratitis
Commonly caused by herpes virus affecting the cornea.
Cornea Transplantation
Required when severe scarring damages vision.
Symptoms of Corneal Ulcer
- Severe eye pain
- Redness in the eye
- Blurred vision
- Excessive tearing
- Discharge from the eye
- Sensitivity to light
- White or gray spot on the cornea
- Swelling of eyelids
Causes of Corneal Ulcer
- Bacterial infections
- Fungal infections
- Viral infections
- Contact lens misuse
- Eye injuries
- Dry eye syndrome
- Immune system disorders
- Vitamin A deficiency
Precautions

Antibiotic / Antifungal Drops
Target infection depending on cause.
Antibiotic / Antifungal Drops
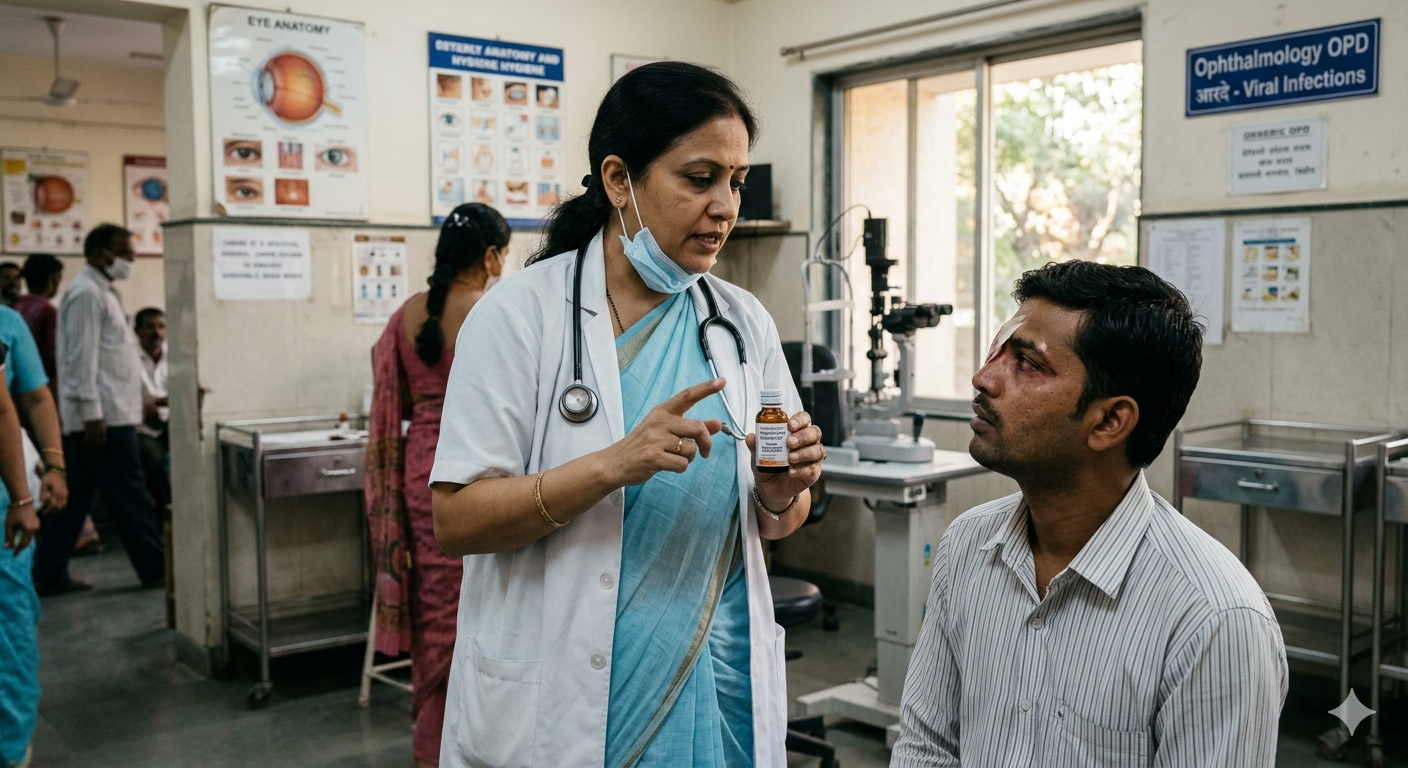
Antiviral Medications
Used in viral keratitis cases.
Antiviral Medications
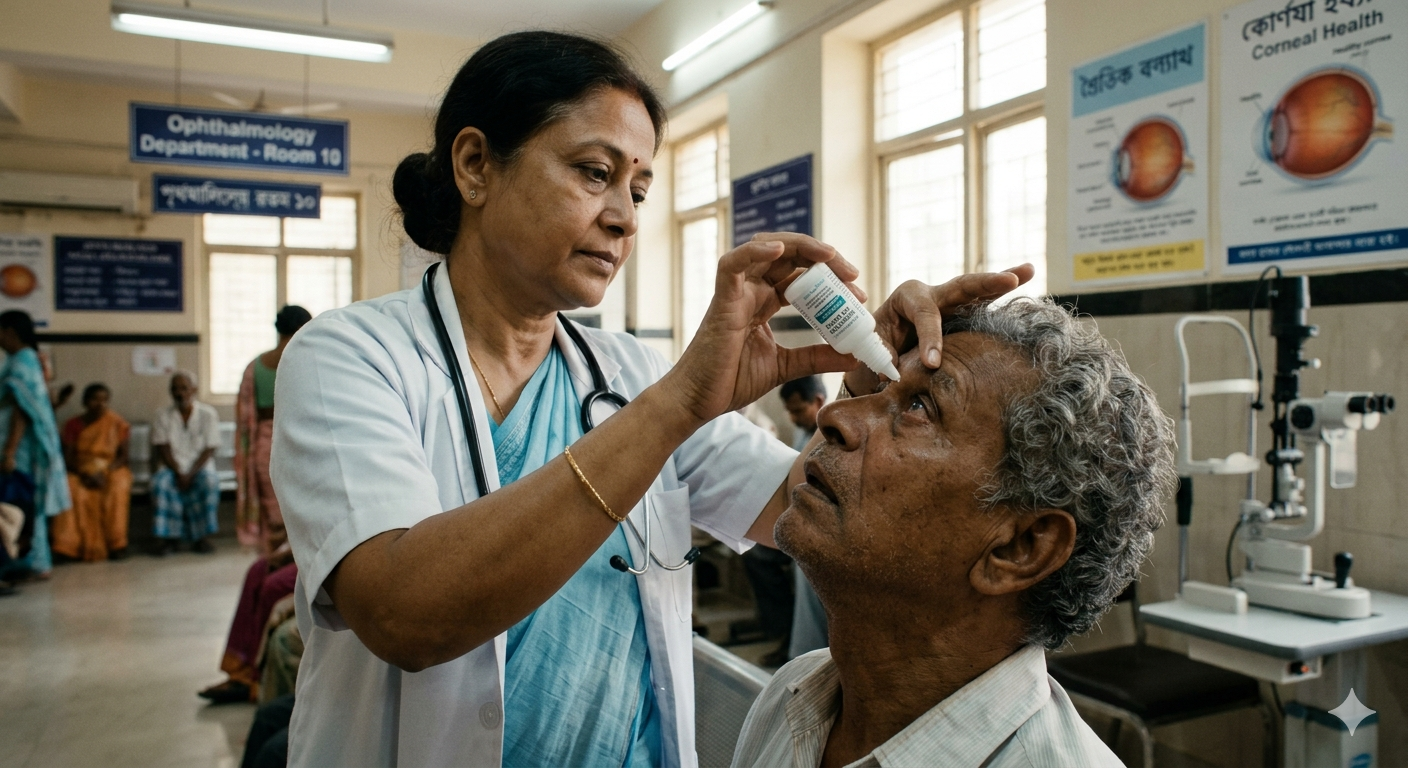
Lubricating Eye Drops
Support corneal healing.
Lubricating Eye Drops

Protective Eye Care
Avoid contact lens use and protect from dust .
Protective Eye Care
Corneal Ulcer Surgery Overview
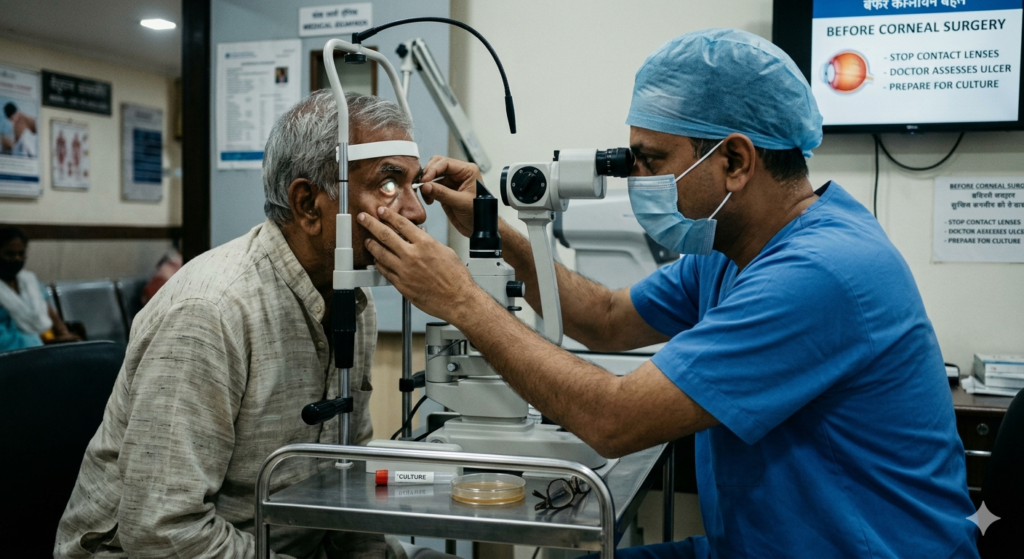
Before Surgery
- Before corneal transplant for perforation, doctor assesses depth and cultures cornea.
- Stop contacts.
- Procedure under local/general anesthesia lasts 30-60 minutes.
- Debridement or glue if small.
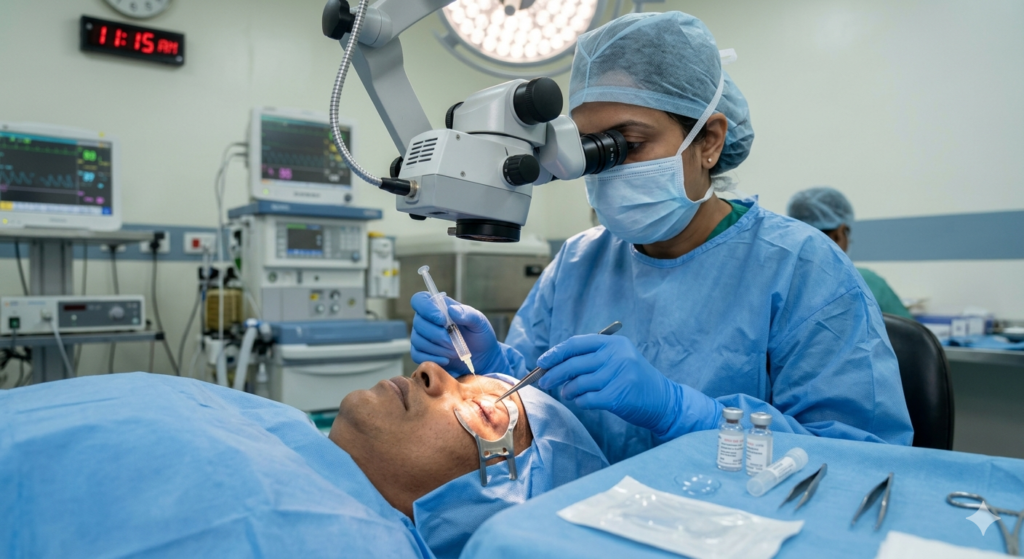
During Surgery
- Awake or sedated.
- surgeon uses cyanoacrylate glue.
- Also uses bandage lens for micro-perforations or therapeutic keratoplasty.
- Punctures sealed.
- Lasts 45 minutes.

After Surgery
- Shield/protective lens.
- Intensive drops taper over weeks.
- Scar forms but vision improves.
- Full re-epithelialization 4-6 weeks.
- Avoid rubbing/water.
- Follow-ups prevent melting.
Treatments of Corneal Ulcer
Therapeutic Penetrating Keratoplasty (TPK)
- It is conventional for perforation.
- Requires full-thickness 7.5-8mm incision.
- Doctor replaces entire cornea in one piece.
- 16-24 sutures required.
- Implants fresh donor tissue.
- It is performed to remove infected or scarred corneal tissue.
The larger incision can sometimes lead to induced astigmatism.
Strict hygiene and medicated eye drops are needed to prevent infection.
Amniotic Membrane Transplant
- It is latest technology.
- Micro-incisional stitchless graft where dehydrated or cryopreserved membrane covers ulcer.
- Placed with fibrin glue or sutures.
- Promotes rapid healing & least scarring with early resolution.
It acts as a natural bandage to protect the corneal surface.
The membrane reduces inflammation and prevents further tissue damage.
It contains growth factors that encourage the growth of healthy cells.
Frequently Asked Questions
Corneal ulcer is open sore on eye’s clear front surface causing pain, redness & vision threat. Common from lenses/trauma, treated intensively with drops/surgery to prevent scarring/blindness.
1. Contact Lenses (Most Common) – Overnight wear, poor hygiene.
2. Trauma – Foreign body/scratch.
3. Dry Eyes – neurotrophic epithelium.
4. Bacterial Infection – Pseudomonas/Staph.
5. Fungal – Agricultural injury.
6. Herpes Virus.
7. Autoimmune (RA/SLE).
8. Steroid Abuse.
9. Vitamin Deficiency.
10. Neurotrophic – Diabetes/after zoster.
Yes it is possible. Stable post-graft LASIK/toric IOL corrects post-ulcer astigmatism/scars for spectacle independence.
1. Impending/Actual Perforation
Iris prolapse, shallow chamber.
Hypopyon worsening.
2. Medical Rx Fails
No improvement 48 hours intensive drops.
3. Other Conditions
Pre-transplant descemetocele.
4. Doctor Advises Surgery
Based on OCT/penlight exam if thinning >80%.
1. Contact Lens Wearers
Extended/poor hygiene highest.
2. Dry Eye Patients.
3. Farmers/Gardeners.
4. Immunosuppressed.
5. Herpes Carriers.
6. Post-LASIK.
7. Rheumatoid Arthritis.
8. Diabetics with neuropathy.
1. Your Vision/Cornea Threatened
Perforation risk imminent.
2. Your Eye Doctor Recommends
Culture-guided no response.
3. You Are Medically Fit
No active sepsis/BP stable.
4. You’re Ready for Post-Op
Intensive drops compliance.
- Proper Contact Lens Care
No tap water, replace cases monthly. - Treat Dry Eyes Aggressively
Punctal plugs, cyclosporine. - Eye Protection
Safety goggles gardening/sports. - Avoid Steroid Self-Medication
Only under ophthalmologist. - Prompt Injury Care
Evert lid, fluorescein stain. - Go for Regular Eye Check-ups
Lens fitters annually, diabetics quarterly.
